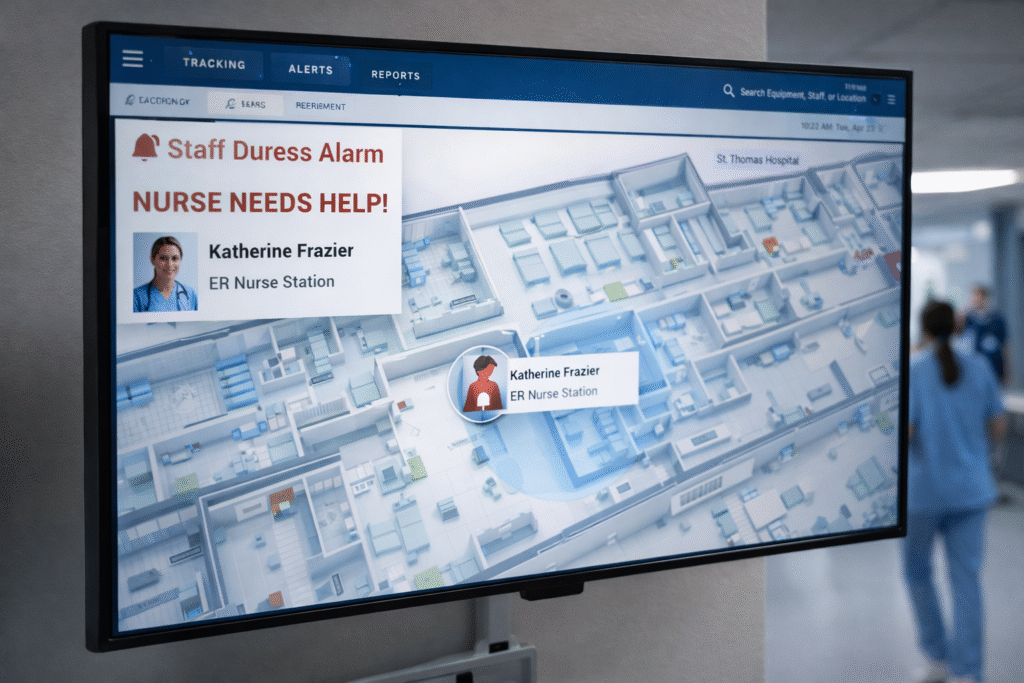
A staff duress system Canada hospitals rely on is a wearable device that allows healthcare workers to silently trigger a real-time, location-specific emergency alert the moment they feel threatened.
According to a 2023 white paper by the Canadian Federation of Nurses Unions (CFNU), healthcare workers experience higher rates of workplace violence than workers in any other sector in Canada.
Still, fewer than half of Canadian hospitals have deployed a real-time staff duress system. The gap between the scale of the problem and the rate of adoption ultimately comes down to one word: cost.
In this guide, we explain how staff duress systems work, what Canadian hospitals should look for when evaluating them, what the law requires, and how costs have changed dramatically in recent years.
Table of Contents
- › What Is a Hospital Staff Duress System Canada Solution?
- › Why Is a Staff Duress System Canada Critical for Hospitals?
- › What Is the Difference Between a Code White and a Staff Duress System?
- › How Does an RTLS-Based Staff Duress System Work?
- › Room-Level Accuracy vs. Sub-Meter Accuracy
- › What Does a Hospital Staff Duress System Canada Cost?
- › What Should Canadian Hospitals Look for When Evaluating a Staff Duress System?
- › Can Small and Mid-Size Canadian Hospitals Afford a Staff Duress System?
- › Are Staff Duress Systems Required by Law in Canadian Hospitals?
- › Frequently Asked Questions
Key Takeaways
- A staff duress system silently alerts security with a worker’s real-time location when the badge button is pressed.
- Over 61% of nurses in Canada report experiencing physical violence on the job (CFNU, 2023), making workplace safety a critical issue across the healthcare system.
- Bill 168 in Ontario and equivalent OHS legislation in BC and Alberta legally require workplace violence prevention programs. Regulators and accreditors now increasingly cite RTLS-based duress systems as the standard of care.
- Legacy systems cost $2M+ for a 200-bed hospital. Newer RTLS platforms bring that figure down to $300K–$500K.
- Room-level accuracy, rechargeable badge technology, and AI-enhanced doorway detection are the three defining features separating modern systems from legacy solutions.
What Is a Hospital Staff Duress System Canada Solution?
A hospital staff duress system Canada providers offer is a technology platform that combines wearable badge hardware, wireless infrastructure, and software to let healthcare workers trigger a silent emergency alert tied to their precise location inside a facility.
Unlike a Code White — a verbal overhead announcement that staff initiate after a situation has already escalated — a staff duress alert is activated the moment a worker senses danger.
The system immediately sends an instant push notification to security and supervisors showing the worker’s name, department, and room location, and updates this data in real time every few seconds.
The system does not make a public announcement. No patient is agitated by an overhead call. Response is faster, more targeted, and more discreet.
Advanced workforce safety platforms use Real-Time Location System RTLS technology combined with Bluetooth Low Energy (BLE) hardware, fixed gateways, and AI-enhanced software. The system delivers room-level or sub-meter location accuracy throughout a hospital campus.
Why Is a Staff Duress System Canada Critical for Hospitals?
Canadian healthcare facilities increasingly view a staff duress system Canada solution as essential due to rising workplace violence. The problem has reached critical levels — regulators, accreditors, and unions now describe it as a crisis.
According to the Canadian Federation of Nurses Unions (CFNU), over 61% of nurses in Canada report experiencing physical violence on the job. Emergency departments, psychiatric units, and long-term care floors are the highest-risk environments, but incidents happen across all units and all shift types.
The regulatory environment has also shifted significantly. The Joint Commission and Canadian accreditation standards now include workplace violence prevention as a required program element.
Bill 168 in Ontario — an amendment to the Occupational Health and Safety Act — legally requires employers to maintain written workplace violence policies and programs that include the ability to summon immediate assistance.
BC’s WorkSafe regulations and Alberta’s OHS legislation carry equivalent requirements. Regulators and accreditors increasingly cite RTLS-based duress systems as the expected standard of care, not an optional upgrade.
For Canadian hospitals, a staff duress system is no longer a best practice. In most provinces, it is a legal and accreditation obligation. For a broader look at how RTLS addresses staff safety alongside other hospital challenges, see our guide on RTLS staff duress in hospitals.
What Is the Difference Between a Code White and a Staff Duress System?
A Code White is a reactive tool.
It is a verbal overhead announcement that the hospital broadcasts facility-wide after a violent incident has already escalated to the point where someone decided to call it in. By the time the announcement plays, the situation is often already critical.
A staff duress system is a proactive, silent, and precise tool.
The worker activates it the moment they sense a threat, before the situation escalates further. Security receives the exact room location without any public announcement that could agitate an already volatile patient or visitor. Response is faster. The worker does not need to speak or make their call for help visible.
The two tools serve different purposes:
Code White remains important for facility-wide coordination.
Staff duress fills the critical gap between a worker sensing danger and a situation becoming a full emergency.
How Does an RTLS-Based Staff Duress System Work?
Modern workforce safety platforms use real-time location technology to enable staff duress alerts and reduce emergency response times. Here is how the end-to-end process works:
Step 1: Badge worn by staff.
Each worker wears a small, lightweight BLE tag clipped to a lanyard or ID holder. The badge continuously transmits a low-energy signal.
Step 2: Gateways receive signals.
The hospital installs fixed gateways throughout the facility. These gateways continuously receive signals from all active badges, mapping each worker’s location in real time.
Step 3: Worker presses badge button.
When a staff member feels threatened, they press the button on their badge. An alert fires through the software platform immediately.
Step 4: Security is notified immediately.
The system sends a push notification to security personnel and supervisors on their mobile device or workstation, showing the staff member’s name, department, and real-time room location — updated every few seconds.
Step 5: The system logs the event.
The system automatically logs every alert with timestamps, location data, and responder actions for compliance reporting, incident documentation, and OHS audit requirements under Bill 168 and equivalent legislation.
Room-Level Accuracy vs. Sub-Meter Accuracy: What Canadian Hospitals Need to Know
Not all RTLS systems provide the same location precision, and the difference matters in a duress scenario.
Room-level accuracy confirms which room a staff member is in with approximately 99% reliability. For most duress situations — where security needs to know the floor and room quickly — this is the practical standard that enables a fast, directed response.
Sub-meter accuracy provides a more granular coordinate, placing the worker within less than one metre. However, sub-meter systems can misidentify the room when a worker is standing close to a shared wall, technically placing them in an adjacent space.
AI-enhanced RTLS systems resolve this limitation by tracking whether the badge has physically passed through a doorway before assigning a room. This doorway-detection logic ensures the system identifies the correct room even in edge cases — delivering the precision of sub-meter technology with the reliability of room-level confirmation.
For Canadian hospital procurement teams, the right question is not simply “how accurate is this system?” but “how does this system handle wall proximity, and what is the false-room-assignment rate?”
What Does a Hospital Staff Duress System Canada Cost?
The cost of a staff duress system Canada hospitals deploy has historically been the primary barrier to adoption, and it remains the most common question procurement teams raise.
Legacy RTLS providers have typically charged $300–$800 per badge. Annual battery replacement costs range from $15,000 to $40,000 for a mid-size hospital. They also require dense gateway infrastructure, which adds hundreds of thousands of dollars in cabling and installation. For a 200-bed hospital, a full legacy deployment could exceed $2 million in total project cost.
A new generation of RTLS providers has restructured the cost model in several important ways:
Rechargeable badges eliminate ongoing battery replacement costs entirely.
Hardware-efficient infrastructure designs reduce the number of gateways required.
Zero-markup hardware pricing removes the traditional vendor margin on physical components.
For a 200-bed Canadian hospital working with a modern RTLS provider, a full staff duress deployment now typically falls in the $300,000–$500,000 range — a reduction of more than 75% compared to legacy solutions. For community hospitals in the 50–150 bed range, the entry point has dropped further still.
The total cost of ownership calculation also shifts significantly when badge battery replacement is eliminated. Over a five-year period, the savings from rechargeable badges alone often exceed the hardware cost difference between legacy and modern systems.
What Should Canadian Hospitals Look for When Evaluating a Staff Duress System?
Choosing the right staff duress system Canada providers offer requires a careful assessment of the following criteria:
Location accuracy — understand whether the system delivers room-level or sub-meter accuracy, and specifically how it handles workers positioned near shared walls.
Badge design — evaluate rechargeable vs. disposable battery models, physical size and discretion for clinical environments, durability for shift-wear conditions, and whether the badge can serve dual purposes such as access control or asset tracking.
Gateway density — the number of gateways required per square foot directly determines installation and cabling cost.
Software integration — confirm compatibility with existing nurse call systems, access control platforms, and EMR infrastructure.
Compliance reporting — verify that the platform can generate incident logs, response time records, and location audit trails suitable for Bill 168 and provincial OHS audit requirements.
Total cost of ownership — evaluate the five-year TCO, not the hardware unit price. Include badge replacement or recharging infrastructure, gateway maintenance, software licensing, and service contract terms.
Vendor implementation experience in Canada — confirm the vendor has deployed in Canadian healthcare environments and understands provincial accreditation and regulatory requirements.
Can Small and Mid-Size Canadian Hospitals Afford a Staff Duress System?
Traditionally, RTLS was considered an enterprise solution viable only for large academic health centres with capital budgets to match. Community hospitals with 50–300 beds were effectively priced out.
That has changed meaningfully. Hardware-efficient infrastructure designs, rechargeable badge technology, and transparent hardware pricing have made RTLS-based staff duress systems accessible to mid-size and smaller Canadian hospitals.
The five-year total cost of ownership for a modern RTLS deployment now frequently compares favourably to older non-RTLS panic button systems, once badge battery replacement and infrastructure maintenance are factored in.
For community hospitals evaluating their options in 2026, the question is no longer whether RTLS is affordable. It is which RTLS model delivers the best long-term value for their specific bed count and facility layout.
Are Staff Duress Systems Required by Law in Canadian Hospitals?
In Ontario, Bill 168 amended the Occupational Health and Safety Act to require employers — including hospitals — to maintain written workplace violence policies and programs that include specific provisions for summoning immediate assistance.
BC’s WorkSafe regulations and Alberta’s OHS legislation carry equivalent requirements.
Beyond legislation, accreditation standards through Accreditation Canada increasingly reference workplace violence prevention technology as a required program component, not an optional enhancement.
RTLS-based staff duress systems are now regularly cited by provincial regulators, OHS auditors, and accreditation reviewers as the expected technological standard for healthcare workplace violence prevention. Hospitals still relying solely on Code White announcements or fixed panic buttons face growing scrutiny during accreditation reviews.
Frequently Asked Questions
What is a staff duress system in a hospital?
A hospital staff duress system is a wearable badge device connected to real-time location software. When a healthcare worker presses their badge button, the system instantly sends a silent alert to security showing the worker’s exact room location. It allows staff to call for help before a situation escalates, without making a public announcement.
What is the difference between a Code White and a staff duress system?
A Code White is a verbal overhead announcement that staff make after a situation has already escalated. A staff duress system is a silent, proactive alert activated by the worker the moment they feel threatened. Security receives the worker’s precise room location without any public announcement that could escalate the situation further.
Are staff duress systems required by law in Canadian hospitals?
Yes, in practical terms. Bill 168 in Ontario requires employers to have workplace violence prevention programs that include means to summon immediate assistance. BC WorkSafe and Alberta OHS legislation carry similar requirements. Regulators and accreditors increasingly cite RTLS-based duress systems as the expected standard of care.
How much does a hospital staff duress system cost in Canada?
Legacy RTLS systems typically cost $2 million or more for a 200-bed hospital when hardware, cabling, installation, and ongoing badge battery replacement are included. Modern RTLS platforms with rechargeable badges and hardware-efficient infrastructure designs have reduced this to approximately $300,000–$500,000 for the same facility size — a reduction of over 75%.
What is room-level accuracy in a staff duress system?
Room-level accuracy means the system can identify which room a staff member is in with approximately 99% reliability. This is the standard required for effective duress response — security receives the correct floor and room instantly. AI-enhanced systems add doorway-detection logic to eliminate false room assignments when a worker stands near a shared wall.
Can a small Canadian hospital afford an RTLS staff duress system?
Yes. The introduction of rechargeable badge technology, hardware-efficient gateway designs, and transparent pricing models has made RTLS staff duress systems accessible to Canadian hospitals with 50–300 beds. The five-year total cost of ownership often compares favourably to older non-RTLS panic button solutions once ongoing battery and maintenance costs are included.
What should I look for when comparing hospital staff duress vendors in Canada?
Evaluate room-location accuracy and wall-proximity handling, badge type (rechargeable vs. disposable), gateway density per square metre, software integration with existing nurse call and EMR systems, compliance reporting for Bill 168 and OHS audits, and five-year total cost of ownership — not just the unit hardware price.
Conclusion
Hospital staff duress systems have moved from optional technology to a clinical, legal, and accreditation requirement for Canadian healthcare facilities.
Provincial OHS legislation requires employers to provide means to summon immediate assistance, and accreditors are tightening their expectations on what constitutes an adequate workplace violence prevention program.
The technology has matured and adoption barriers have decreased. RTLS platforms now deliver room-level accuracy with AI-enhanced doorway detection. Rechargeable badge technology has eliminated one of the largest ongoing cost drivers. Hardware-efficient infrastructure designs have brought total project costs within reach of community hospitals that were priced out of the market five years ago.
For Canadian hospitals evaluating their options in 2026, the question is no longer whether to deploy a staff duress system. It is how to choose the right platform — one that delivers accurate location data, meets provincial compliance requirements, and delivers long-term value at a cost that reflects how significantly this market has changed.
Ready to Protect Your Healthcare Workers?
Whether you are preparing an RFP for a staff duress system, evaluating vendors, or need guidance on Bill 168 compliance — our team is ready to help.